Skin Cancer Removal Surgery / Mole Removal
(Basal Cell Carcinoma, Squamous Cell Carcinoma, Melanoma)
Here in sunny South Florida, it is important to be vigilant for signs of skin cancer. If you have a skin lesion which causes you concern, please contact Dr. Berens immediately at 954-916-1100 to set up an appointment.
Skin cancer is the most common form of cancer in the USA. More than 500,000 new cases are reported each year-and the incidence is rising faster than any other type of cancer. While skin cancer can be found on any part of the human body, the cast majority appear on the head, face or neck, where they can be disfiguring as well as very dangerous.
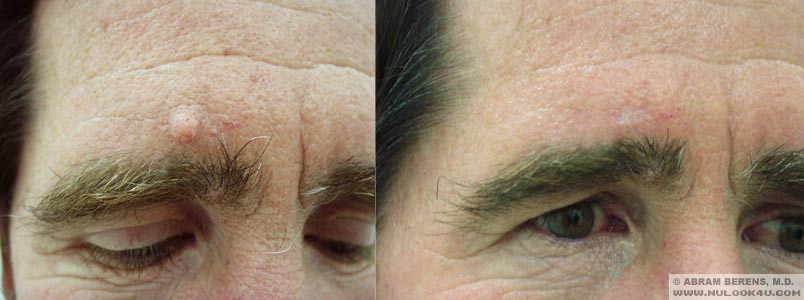
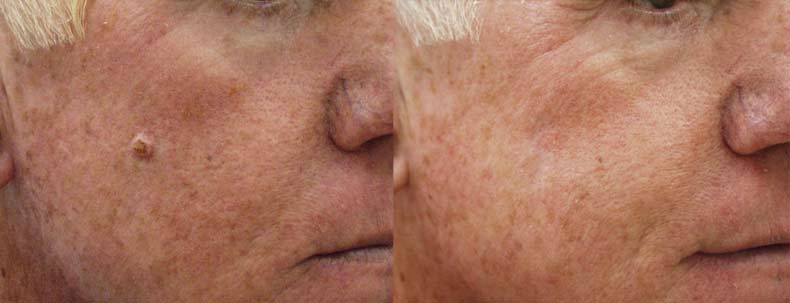
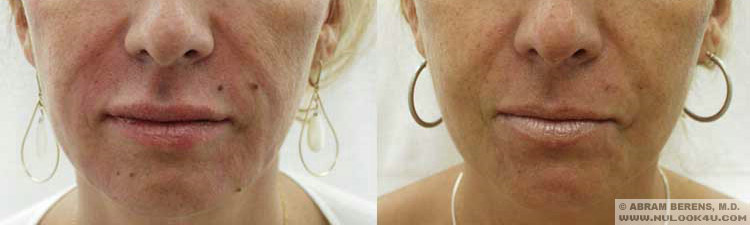
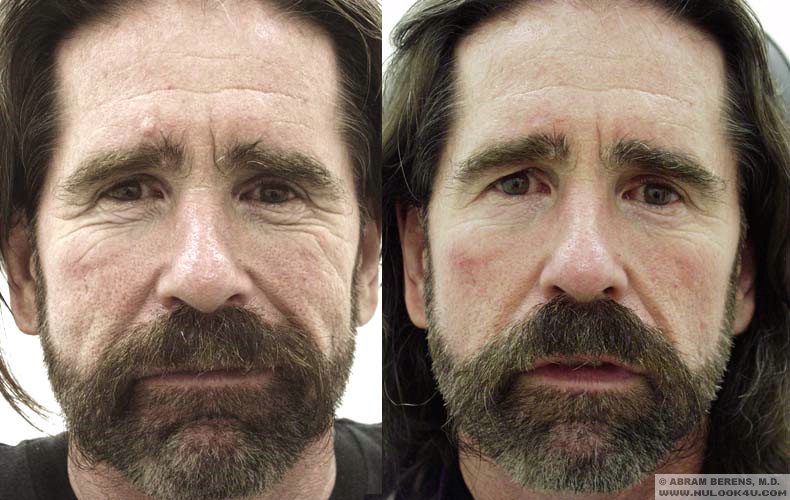
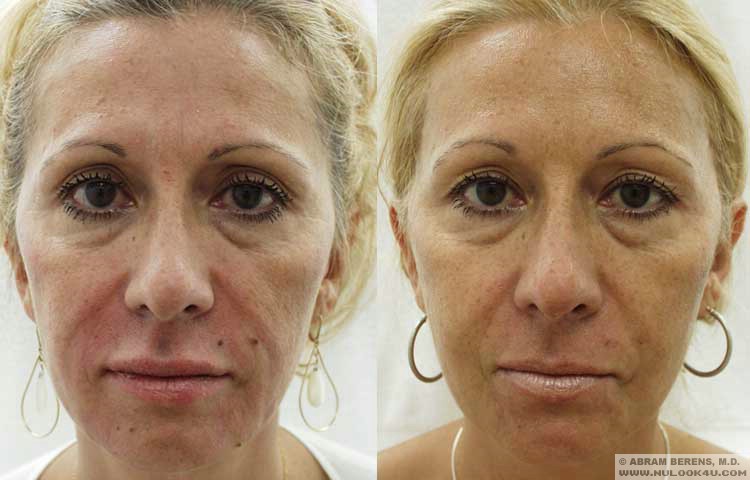
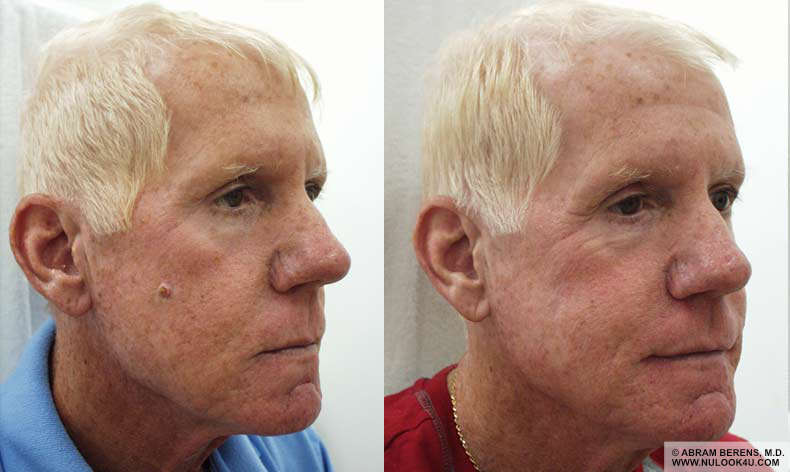
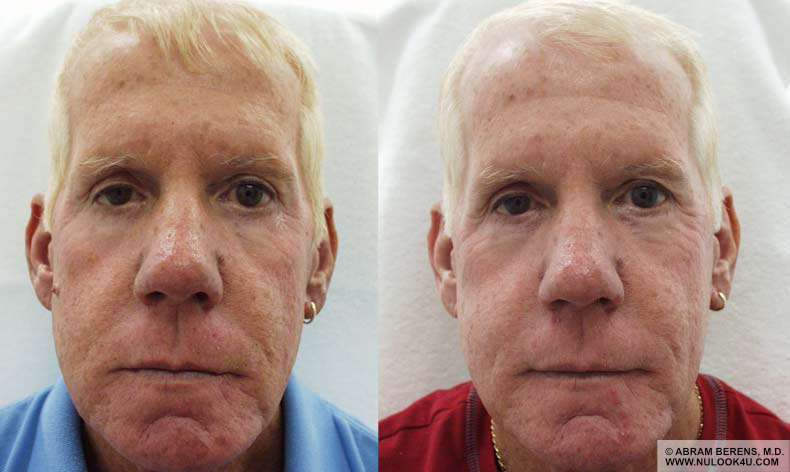
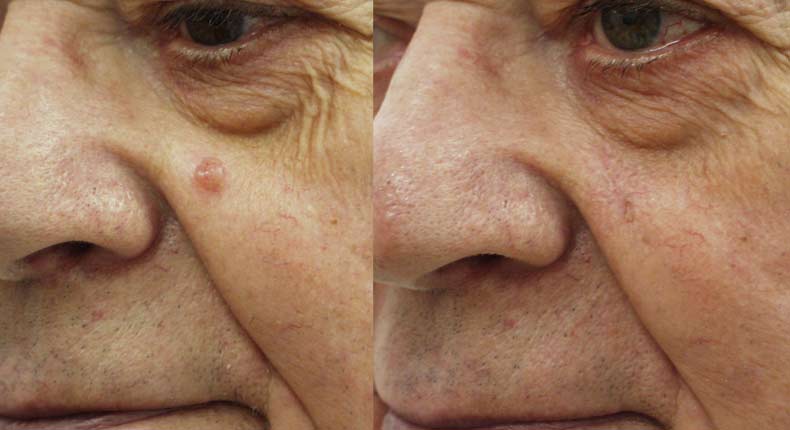
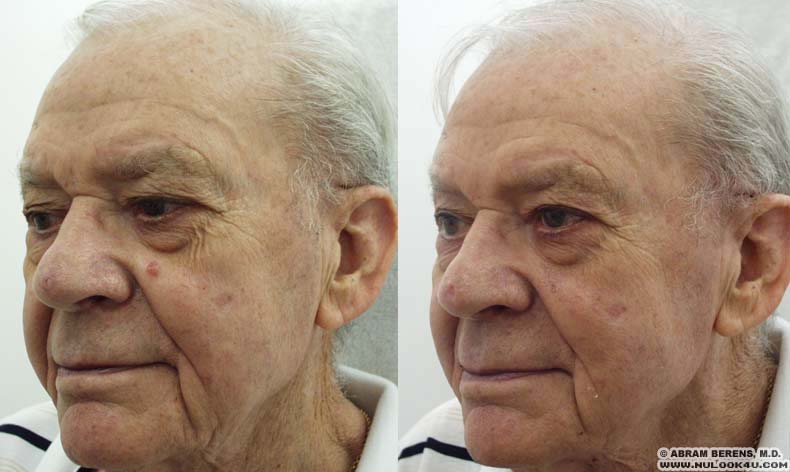
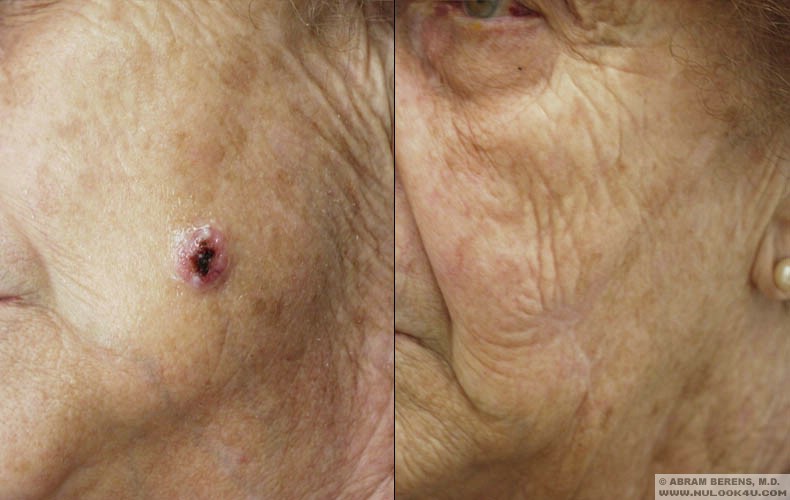
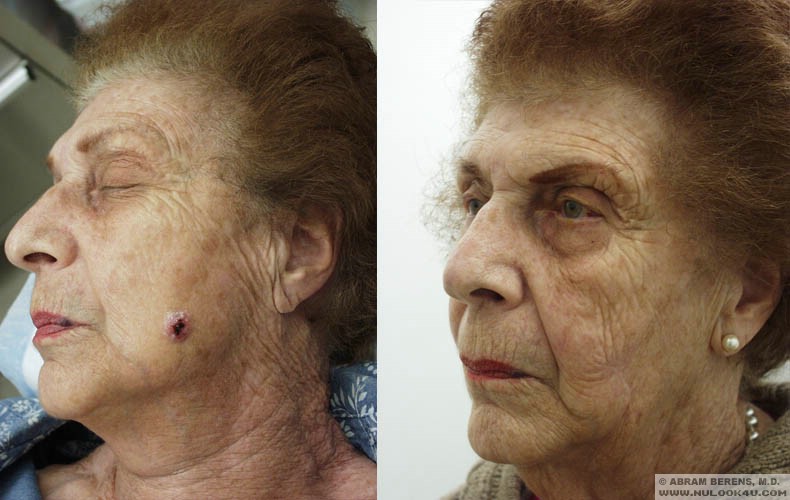
Before and After Photos